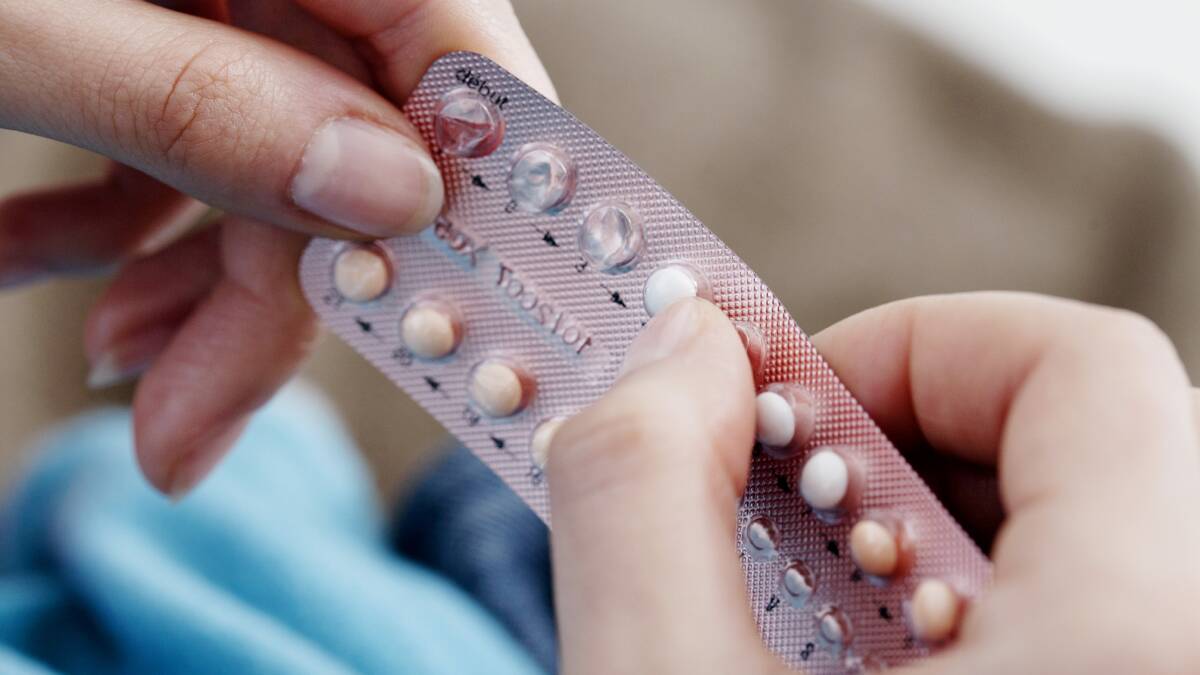
A Ballarat 29-year-old has shared her experience finding out she has fertility issues in the hopes more young women will seek the information they need to plan ahead if they wish to have children.
Subscribe now for unlimited access.
or signup to continue reading
Behaviour Support Practitioner Sarah Oakley was diagnosed with polycystic ovarian syndrome (PCOS) in 2022 and says knowing more about the condition earlier would have given her more time to weigh up her options.
The diagnosis came after Sarah stopped taking the oral contraceptive pill and noticed she was not getting a period.
Her GP initially brushed off her fertility concerns, based on her young age, but she insisted on further examination.
Blood tests showed a slight abnormality in her hormone levels. But it wasn't until she got a referral to a gynaecologists' for an ultrasound she found her ovaries were, in her words, "cooked".
"The gyno had a student with him at the time and he just pointed to [the ultrasound] and said, 'You've probably got a picture in your textbook of what PCOS looks like, and it probably looks exactly like that', " Sarah said.
The advice was if Sarah wanted to try for a baby, she "shouldn't bother" without coming back to the doctor's office for fertility treatment first.
The news came as a shock, as Sarah had experienced monthly withdrawal bleeding as expected while on the pill, and so assumed she had been ovulating as normal.
She had no idea the pill and other hormonal contraception could "mask" fertility issues in such a way.
She thinks someone may have told her once in her younger years, but until her diagnosis, she'd had no reason to suspect that's what was happening.
"It had never occurred to me that a withdrawal bleed was just that - it wasn't an actual period, it was artificial and had nothing to do with my actual cycle," she said.
"It wasn't until I stopped taking [the pill] completely, and didn't have a period for months and months, that I was like, 'oh hang on, things are not working'."
Sarah counts herself "lucky" having children is not a priority for her at this point in her life, as she knows how distressing fertility struggles can be for many women who are wanting to become mothers.
For those who may be thinking about planning for a baby, she hopes sharing her story will encourage women to "get to know their bodies" sooner rather than later, as well as help normalise the fact pregnancy is not always going to happen according to the desired schedule.
"A lot of the time you don't know [there might be a problem] until you're ready to start trying and by that point, you might've made decisions around partners or houses or career choices," she said.
"I know people who've put off changing careers or getting a job or a qualification because they're thinking 'the next step for me is becoming a parent'.
IN THE NEWS
"They've put everything else off and then find out that it's not going to happen as quickly as they would hope."
"I don't know how or when I would've thought, 'maybe I should check if I'm actually fertile' - the thought had never entered my mind that I might not be," she said.
"I didn't even have the concept in my mind that it would be something that would not happen without intervention."
Based on her experience, Sarah's advice is to speak to a GP first about any concerns, and "speak to your mum if you're able to as well".
"Find out what her experience was with fertility - maybe she had a perfect cycle and popped out kids exactly on schedule, maybe that was absolutely not the case and she just hasn't spoken to you about it.
"Obviously, not everyone can do that or is comfortable to do that but it's just about arming yourself with as much information as you can about your own history and your own likelihood of what that might look like for you."
Polycystic ovarian syndrome (PCOS)
- Affects up to 1 in 10 girls and women in their reproductive years.
- The cause is not fully understood, however family history and genetics, hormones and lifestyle play a role.
- May cause disruptions to the menstrual cycle, skin and hair changes, as well as cysts on the ovaries.
- Is one of the leading causes of infertility, yet many women don't know they have it.
- Can't be cured, but if you have it you and your doctor can manage many of the symptoms.
Sources: healthdirect.gov.au, betterhealth.vic.gov.au.
Have you signed up to The Courier's variety of news emails? You can register below and make sure you are up to date with everything that's happening in Ballarat.

